Cannabis Addiction
Cannabis is addictive
Most people who use cannabis don’t get addicted to it or experience harm. However, it’s a myth that cannabis is not addictive. Cannabis addiction, also called Cannabis Use Disorder (CUD), is a condition that impairs social functioning, decision-making, and school/work performance.
There is significant risk of developing cannabis addiction among people who use frequently
Cannabis is the most-used drug after alcohol and tobacco in the United States. Recent polls show that cannabis use is beginning to overtake tobacco use to become the second most used drug nationwide.
- About 9-30% of people who start using cannabis will become addicted.8-11 Data suggests that 30% of heavy cannabis users may have some degree of cannabis use disorder.6
- In 2022, about 19 million people in the United States met the criteria for cannabis use disorder. Most (55%) had a mild disorder, however more than 3 million people (17%), met criteria for a severe disorder.1
- Using cannabis more often (especially daily) and using products with high concentrations of THC increases the likelihood of developing a cannabis use disorder.2-5
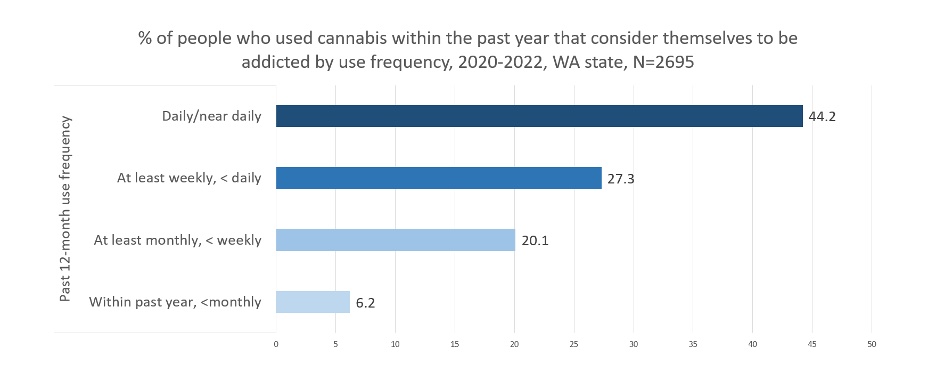
In Washington State, 27.6% of people who used cannabis in the past year considered themselves to be addicted. And almost half of all people who used daily (or near daily) considered themselves addicted.12
Cannabis use disorder symptoms
Cannabis use disorder can happen when people continue using cannabis despite experiencing related problems. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) describes 11 criteria used to diagnose all substance use disorders, including cannabis use disorder. Even though these 11 criteria are the same for all substances, the severity of consequences is not the same. For example, opioid use disorder is related to high death rates, while cannabis use disorder is extremely unlikely to lead to death.
The severity of a person’s disorder is determined by the number of criteria they meet. People who meet two or three of the criteria are considered to have a mild disorder, while people who experience six or more symptoms are considered to have a severe disorder.
These symptoms can be grouped into four general themes:
- Social Problems. Having arguments with family or friends, or not engaging in school, work, responsibilities at home, or hobbies.
- Impaired control. Using more often or more than wanted, craving cannabis in between use, not being able to stop using, or spending a lot of time getting, using or recovering from use.
- Risky Use. Using in situations that may not be safe (like while driving), or continuing to use even when use makes physical or mental health problems worse.
- Physical dependence. Needing more or stronger cannabis to get the same effect, or experiencing withdrawal symptoms in the week or so after stopping use.
WITHDRAWAL SYMPTOMS
- Anger, irritability, or aggression
- Nervousness or anxiety
- Restlessness
- Decreased appetite
- Depression
- Not being able to sleep
- Having strange dreams
- Headaches, nausea, vomiting, sweating or abdominal pain
- Tremors, in some cases
Treatments for cannabis use disorder
Evidence based behavioral therapies exist to treat cannabis use disorder. Some, such as Motivational Enhancement Therapy (MET), focus on helping people identify how their use helps or gets in the way of personal goals. Others, such as Cognitive Behavioral Therapy (CBT) and Contingency Management (CM) teach behaviors that help people reduce use or quit, and offer rewards when goals are met. Many treatment providers combine more than one type of behavioral therapy when working with patients. Some people have found help by going to 12-step programs and mutual help support.
In addition, several treatments focus specifically on teen substance use and involve families and caregivers. These include the Adolescent Community Reinforcement Approach (ACRA), Functional Family Therapy (FFT), and Multidimentional Family Therapy (MDFT).
Right now, there are no FDA-approved medications to treat cannabis use disorder, but research in this area is underway.
Here are some online tools for people wanting to quit or reduce their cannabis use:
- The University of Vermont has designed and tested T-Break: Take a Cannabis Tolerance Break, a 21-day guide on taking a cannabis break.
- What’s the Deal on Quitting? A Do-It-Yourself Guide to Quitting Cannabis is a 20 page PDF from the Australian National Cannabis Prevention and Information Centre designed to help you make changes to your cannabis use and manage the kinds of challenges you may face in the process. It can be used as a tool to help you reduce your use or quit completely.
If you or someone you know needs help with their cannabis use, visit our Get Help page for a list of helplines, tools and resources.
References
- SAMHSA (2022). Highlights for the 2022 National Survey on Drug Use and Health. https://www.samhsa.gov/data/release/2022-national-survey-drug-use-and-health-nsduh-releases
- Bidwell LC, YorkWilliams SL, Mueller RL, Bryan AD, Hutchison KE. Exploring cannabis concentrates on the legal market: User profiles, product strength, and health-related outcomes. Addictive Behaviors Reports. 2018;8:102-106.
- Curran HV, Hindocha C, Morgan CJA, Shaban N, Das RK, & Freeman TP. Which biological and self-report measure of cannabis use predict cannabis dependency and acute psychotic-like effects? Psychological Medicine. 2019;49:1574-1580.
- Hines LA, Freeman TP, Gage SH, Zammit S, Hickman M, Cannon M, Munafo M, MacLeod J, & Heron J. Association of high-potency cannabis use with mental health and substance use in adolescence. JAMA Psychiatry. 2020;epub ahead of print E1-#8.
- Freeman TP, & Winstock AR. Examining the profile of high-potency cannabis and its association with severity of cannabis dependence. Psychological Medicine. 2015;45:3181-3189.
- Hasin DS, Saha TD, Kerridge BT, et al. Prevalence of Marijuana Use Disorders in the United States Between 2001-2002 and 2012-2013. JAMA Psychiatry. 2015;72(12):1235-1242. doi:10.1001/jamapsychiatry.2015.1858.|
- Winters KC, Lee C-YS. Likelihood of developing an alcohol and cannabis use disorder during youth: Association with recent use and age. Drug Alcohol Depend. 2008;92(1-3):239-247. PMCID: PMC2219953
- Anthony JC, Warner LA, Kessler RC. Comparative epidemiology of dependence on tobacco, alcohol, controlled substances, and inhalants: Basic findings from the National Comorbidity Survey. Exp Clin Psychopharmacol. 1994;2(3):244-268.
- Lopez-Quintero C, Pérez de los Cobos J, Hasin DS, et al. Probability and predictors of transition from first use to dependence on nicotine, alcohol, cannabis, and cocaine: results of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC). Drug Alcohol Depend. 2011;115(1-2):120-130. PMCID: PMC3069146.
- Anthony JC. The epidemiology of cannabis dependence. In: Roffman RA, Stephens RS, eds. Cannabis Dependence: Its Nature, Consequences and Treatment. Cambridge, UK: Cambridge University Press; 2006:58-105
- Hall WD, Pacula RL. Cannabis Use and Dependence: Public Health and Public Policy. Cambridge, UK: Cambridge University Press; 2003.
- Corsetti D, Fataar F, Burkhalter R, Rynard V, Hammond D. International Cannabis Policy Study Code Book – Wave 5 (2022). Univeristy of Waterloo; Waterloo, ON, Canada. September 2022. http://cannabisproject.ca/methods/
- McNeely J, Adam A. Substance Use Screening and Risk Assessment in Adults [Internet]. Baltimore (MD): Johns Hopkins University; 2020 Oct. Table 3, DSM-5 Diagnostic Criteria for Diagnosing and Classifying Substance Use Disorders [abc].
Last updated January 2024.
